Juvenile Dermatomyositis
Juvenile dermatomyositis (JDM) is a rare inflammatory muscle disease of childhood that can present at any age. It is characterised by typical skin changes and proximal muscle weakness, with a wide range of severity.
Clinical features
- Skin features:
- Malar rash
- Heliotrope rash (violaceous rash over the eyelids)
- Photosensitivity
- Vasculitic skin changes
- Nailfold capillary changes
- Gottron’s papules over the knuckles, elbows or knees
- Musculoskeletal and muscle features:
- Proximal muscle weakness (e.g. difficulty climbing stairs or rising from sitting)
- Myalgia
- Arthritis or arthralgia
- Joint contractures
- Other features:
- Malaise, fever, weight loss or anorexia
- Dysphagia or dysphonia
- Dyspnoea (including interstitial lung involvement)
- Bulbar or chest wall muscle weakness with risk of aspiration pneumonia
- Skin ulceration or oedema
- Calcinosis (calcium deposits under the skin)
Diagnosis
Diagnosis is based on clinical assessment supported by investigations. Typical findings include elevated muscle enzymes (e.g. CK, AST, ALT, LDH) and MRI of affected muscles to confirm inflammation and monitor disease activity.
Muscle biopsy may show inflammation, fibre necrosis and small vessel vasculitis but is not routinely required if the clinical picture is typical. Electromyography is rarely used.
It is important to consider inherited myopathies, which can also present with elevated muscle enzymes. Unlike adult-onset dermatomyositis, JDM is not typically associated with malignancy and routine cancer screening is not required.
Disease course and complications
- Calcinosis
- Interstitial lung disease
- Gastrointestinal vasculitis
- Growth and functional impairment
- Associated arthritis
Management
Management requires specialist multidisciplinary care. Treatment commonly includes high-dose corticosteroids (often initially intravenous) and methotrexate as a steroid-sparing agent.
In more severe or refractory disease, additional treatments may include intravenous immunoglobulin (IVIG), cyclophosphamide and biologic therapies.
Physiotherapy and rehabilitation are essential to optimise muscle strength, function and long-term outcomes.
Clinical approach
Early recognition and prompt referral are important to prevent long-term complications, including calcinosis and functional disability.
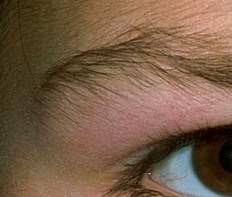
The photograph below shows characteristic heliotrope rash over the eyelid
The photograph shows calcinosis in JDM

The photographs below shows typical Gottron's papules over the knuckles in JDM



