Tuberculosis
Clinical features
Tuberculosis (TB) in children often presents with a swollen joint, although the joint may not be hot or erythematous. The course is typically indolent, which can lead to delayed diagnosis. Inflammatory markers are usually raised, and anaemia of chronic disease may be present. The spine is a common site (Pott’s disease), where vertebral collapse may result in kyphosis or paraplegia. Other frequently affected sites include the femur, tibia, skull, and small bones of the hands and feet. Dactylitis may occur, presenting as painless or mildly painful swelling of the proximal phalanges or metacarpals.
Atypical mycobacteria
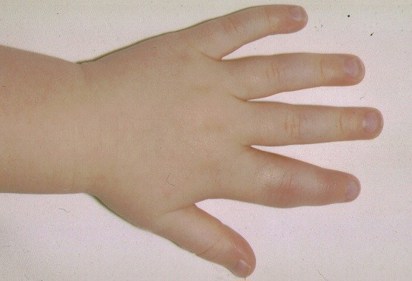
Atypical mycobacterial infections may be acquired from environmental exposure, including contact with pets such as reptiles or tropical fish. These infections are typically indolent and may involve the skin, soft tissues or joints.
Special forms
Poncet’s disease is a reactive arthritis thought to represent hypersensitivity to tuberculoprotein. It presents with fever followed by an acute or subacute symmetrical oligoarthritis, usually affecting large joints such as the knees, and is commonly associated with active extra-pulmonary TB, particularly lymph node disease. Cervical or axillary lymphadenopathy is a consistent feature, and the arthritis typically resolves with anti-tuberculous therapy. Phlyctenular conjunctivitis (phlycten) is an allergic eye condition that may also indicate underlying mycobacterial infection.
Diagnosis
Diagnosis is based on a combination of clinical suspicion, history and investigations. Important clues include TB contact history, systemic symptoms, and characteristic imaging findings. Investigations may show lymphocytic leucocytosis and raised ESR, and a Mantoux test is often positive. Radiographs may demonstrate bony collapse or lytic lesions, while MRI is particularly sensitive for spinal disease. Definitive diagnosis requires culture from bone or synovial tissue, and molecular testing (PCR/DNA analysis) may provide more rapid results where available. In regions where multidrug-resistant TB is prevalent, culture and sensitivity testing are essential. The differential diagnosis includes septic arthritis, fungal infection, bone tumours and juvenile idiopathic arthritis.
Differentiating TB, septic arthritis and JIA
|
Feature |
Mycobacterial / TB |
Septic arthritis |
Juvenile idiopathic arthritis |
|
History |
TB contact may be present; often monoarthritis; spine involvement common |
Acute onset, severe pain, febrile child |
Variable; may have rash or uveitis |
|
Pattern |
Monoarthritis typical; extra-articular features; Mantoux often positive |
Monoarthritis, any joint |
Variable pattern; >6 weeks duration |
|
Systemic features |
May have systemic symptoms and lymphadenopathy |
Systemically unwell, febrile |
Variable systemic features |
|
Laboratory tests |
Lymphocytic predominance; ESR raised |
High WCC, raised ESR/CRP |
May have normal or mildly raised markers |
|
Synovial fluid |
Raised WCC; culture may grow mycobacteria; granulomas on biopsy |
Very high WCC; organisms cultured |
Moderately raised WCC; sterile fluid |
Key points for healthcare professionals
- Always consider tuberculosis in a child with chronic monoarthritis or spinal disease
- Dactylitis in a young child may be a marker of TB
- Remember Poncet’s disease as a cause of reactive arthritis in the context of active TB
- Culture and sensitivity testing are essential to guide treatment
- Differentiation from septic arthritis and JIA is critical for safe management
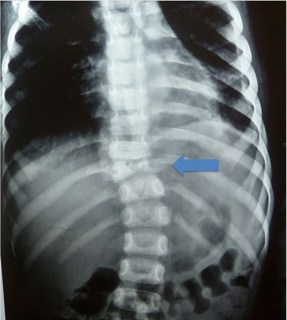
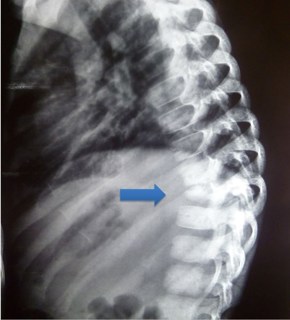
The radiographs below show vertebral collapse (arrowed) due to TB of the spine.
The photograph below shows a swollen index finger involving the proximal interphalangeal joint and due to atypical mycobacteria, in a child on immunosuppressive treatment.