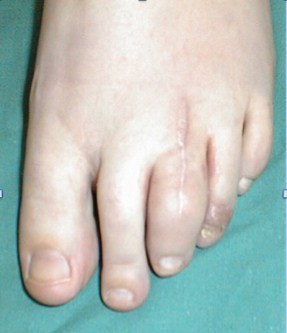
Swollen toe
Jordan is a 15 year old boy who presents with a swollen toe to accident and emergency.
He is a keen footballer but cannot recall any injury. Otherwise he is well with no systemic features to suggest red flags in the history and the examination is otherwise reported as normal from the emergency department assessment. He has a swollen toe ('sausage like').
Investigations - radiograph shows no fracture. Ultrasound shows soft tissue swelling and effusion in the interphalangeal joint and metatarsal joint. Full [complete] blood count, acute phase reactants normal. Autoantibodies are normal.
He is referred to orthopaedics who perform aspiration of the toe joint under anaesthetic. Cultures are negative but he has a six week course of antibiotics.
At review, he is no better and now has pain in his fingers. He is referred to paediatric rheumatology.
pGALS demonstrates small joint involvement in his fingers and nail pitting. There is a family history of psoriasis (father).
The diagnosis is Juvenile Psoriatic Arthritis (JPsA).
The involvement of small joints, often in an asymmetrical pattern, is typical of JPsA. The skin and nail changes may be absent or very mild. It is important to assess the nails in the hands and feet. Subtle skin changes may be found (scalp, natal cleft, umbilicus). The family history is helpful when the skin and nail changes are absent. It is important to assess all joints as it is not uncommon to detect joint involvement that is 'silent' - pGALS is useful to perform a quick screen of all joints.
There is risk of uveitis with JPsA and this is often without symptoms in the early stages (i.e., no redness, pain or blurring).
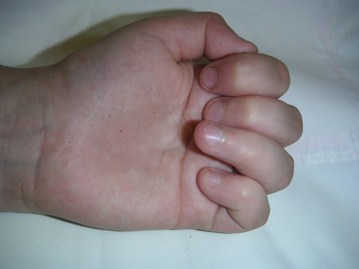
The photograph below shows restricted full flexion of the left ring finger distal interphalangeal joint in a child with JPsA.
Jordan had Joint injections under general anaesthetic.
He was started on subcutaneous methotrexate (MTX) and folic acid. He was taking NSAIDS for pain relief.
Input from the multidisciplinary team included education about his condition and treatment. The family were taught how to administer MTX at home with weekly injections. He had outpatient physiotherapy.
Slit lamp examination showed no uveitis and he had regular eye screening.
His arthritis settled and he was in remission at the 3 monthly review in the outpatient clinic.
He was able to attend school full time and take part in sports.
The picture below shows a swollen toe with a well healed scar from previous surgery.