Swollen Joint
A two year old girl is referred to clinic with an eight week history of a swollen right ankle (photograph below). Her parents have noticed that she is asking to be carried more often but she remains generally well. pGALS demonstrates no joint involvement elsewhere but she has calf wasting (right side) (photograph below).
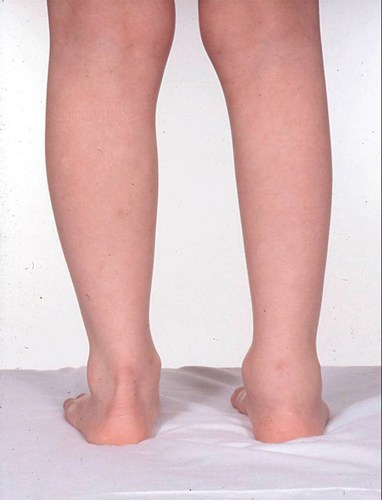
Differential diagnosis
This little girl is likely to have oligoarticular JIA but the history, physical examination, and/or initial investigations must exclude other possible diagnoses, including septic arthritis, Tuberculosis arthritis, Acute Rheumatic Fever (although more likely to be a migratory 'flitting' polyarthritis) and malignancy.
Red flags would include systemic upset (such as fever, weight loss, night pain, pallor, lymphadenopathy, bone tenderness). The presence of calf wasting suggests chronicity and in the presence of a well child, suggests that JIA is more likely.
Full [complete] blood count: This should be normal in a child with oligoarticular JIA and one swollen joint. A low haemoglobin, low white cell count or platelets should raise the possibility of haematological malignancy such as leukaemia and further investigations including blood film and bone marrow aspirate may be required. Significantly elevated neutrophil or platelet counts may indicate underlying infection.
Acute phase reactants: Significantly elevated acute phase reactants (ESR or CRP) are unusual in oligoarticular JIA and should trigger further investigations to exclude infection (including acute rheumatic fever, reactive arthritis) and / or malignancy.
Infection screen: Investigations pending the clinical context include blood cultures, serology (e.g., ASOT) or throat swab. Synovial fluid aspiration is required for a single swollen joint and infection excluded. Tuberculosis [TB] needs to be considered and excluded (chest radiograph, Tuberculin skin testing or QuantiFERON® testing). Human Immunodeficiency Virus (HIV) may coexist with TB. Other infections need to be considered pending the location or travel history (e.g., arbovirus transmitted infections [Lyme disease, Chikungunya, Dengue] or Brucellosis).
Anti-nuclear antibody (ANA): A positive ANA can occur in JIA and is associated with an increased risk of uveitis. Although all children with JIA are at risk from uveitis, young children, particularly girls, with persistently positive ANA are at higher risk. ANA is not diagnostic of JIA, can be observed in normal healthy children or with intercurrent illness.
Slit Lamp Examination: Prompt referral for eye screening is needed as she may have chronic anterior uveitis, whether she is ANA positive or not. She is at high risk of chronic anterior uveitis given her age, and clinical presentation.
Rheumatoid factor: RF is unlikely to be positive in children with oligoarticular JIA.
HLA-B27: There are HLA associations for each JIA subtype, particularly important in oligoarticular disease. HLA-B27 plays an important role in the classification of JIA and is associated with both enthesitis related arthritis and psoriatic arthritis. HLA-B27 positivity predicts more aggressive disease and the likelihood of acute uveitis with a painful red eye. HLA-B27 is useful in the assessment of the older child with peripheral arthritis predominantly involving the lower limb or in the presence of enthesitis or sacroiliitis.
Plain radiograph: May show erosive disease in late presentations but usually radiographs will be normal in early presentation of JIA. Radiographs are indicated if there is any suggestion of physical trauma. If non-accidental injury is suspected then a skeletal survey may be needed to look for injuries elsewhere (e.g., ribs, long bones).
Ultrasound scan (USS): If available, then USS can be very useful in determining the presence of sub-clinical synovitis and/or tenosynovitis.
Magnetic Resonance Imaging (MRI): May be useful in children with unusual presentations or long-standing disease in which it can be difficult to differentiate between damage and active synovitis. MRI is very useful where joints are less accessible (such as hips, shoulders, sacroiliac joints), or where there is clinical uncertainty (such as ankle, subtalar joints) or to exclude other diagnoses (e.g., meniscal injury, pigmented villonodular synovitis, tumour).


