Fever & Arthritis
Poppy is 9 years old and has a 3 week history of pain in her legs and intermittent limp. Blood tests taken by her local doctor were normal. She deteriorated over a weekend with high fever, rash, sore throat and joint pain.
She was admitted to her local hospital. Blood tests showed high acute phase reactants (CRP 200mg/L, ESR 70mm/hr). Throat swab was negative but AntiStreptolysin (ASO) Titre was high. Blood cultures were negative. She was started on IV antibiotics but referred to paediatric rheumatology in view of recurrent fever (often in the evening) with rash. Her joints were normal, there was no splenomegaly but a few small cervical lymph nodes were palpable. Repeat blood tests showed high CRP (120), ESR (98) serum ferritin high (1500ng/L), anaemia (Hb 8) and a normal blood film. The titre of ASOT was unchanged and anti-DNAse B was not elevated when checked 10 days later.
She was reviewed by haematology and a bone marrow was performed (reactive inflammatory changes only). After several days of antibiotics, she remained unwell with recurrent fever, rash and developed joint pain (hips, knees, hands and wrists, shoulders).
This is Systemic onset JIA.
- The diagnosis is made by exclusion - infection (especially Tuberculosis [TB] or acute rheumatic fever in high risk populations) and malignancy need to be considered and excluded.
- The presentation of SOJIA can be indolent or acute. The arthritis may not be apparent at first but may follow 4-6 weeks after the onset of systemic symptoms.
- Bone marrow may need to be considered to exclude malignancy (leukaemia or neuroblastoma). The peripheral blood film may not show blasts with acute leukaemia.
- It is important to exclude malignancy (leukaemia) before starting corticosteroids as the survival from leukaemia is much worse with only corticosteroid pre-treatment. It is important to consider a bone marrow if there are atypical features such as a low or normal platelet count (platelets are usually very high with SOJIA). A bone marrow may be needed to exclude malignancy (leukaemia or neuroblastoma); the peripheral blood film may not show blasts. In this case the child was unwell, the ferritin was very high and there was no apparent arthritis.
- Bone marrow can also aid in the diagnosis of infections such as TB.
- Chest X-ray and TB skin testing should be performed and other infections such as Malaria or Arboviruses should be considered in endemic areas or if there is a relevant travel history.
- If there is evidence of streptococcal infection with positive throat swab culture (supportive evidence), or evidence of past infection with highly elevated or rising streptococcal titres (definitive evidence) then Rheumatic fever must be considered. The arthritis usually affects large joints, is usually migratory and very responsive to NSAID treatment. Inflammatory markers are elevated (ESR >50 and CRP >30 meets the ARF diagnostic criteria. Careful cardiac examination (for a murmur), an ECG for PR interval and ECHO should be arranged. High risk patients include Maori and Pacific and/or those living in overcrowded situations.
She was treated with IV corticosteroids, daily over 3 days, improved rapidly and discharged home on oral steroids to be reviewed after one week. She returned with more joint pain, recurrence of rash and fever. She had polyarthritis.
She was given further course of IV corticosteroids over 3 days and started on methotrexate weekly and discharged on oral steroids to be reviewed for blood tests in 4 weeks. Patients are increasingly started on subcutaneous methotrexate as this is likely more effective and often better tolerated with less nausea; clinical practice however varies around the world - patients may be started on oral methotrexate.
The family attended weekly to meet the nurse and taught how to safely store and administer methotrexate at home. At her 4 week review she was well but had ongoing arthritis, intermittent rash but no fever. She was intolerant of methotrexate (now being given by subcutaneous route), even with antiemetics. After discussion with her family she was started on tocilizumab (IV infusion on the day unit) every fortnight and was able to continue lower dose of subcutaneous methotrexate. After 3 months she was well, in remission and had stopped her steroids. She attends the day unit for infusions of tocilizumab.
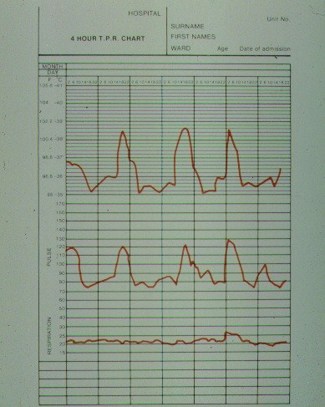
The chart shows the typical fever chart - spikes in the evening but normal in between. The typical maculopapular rash often appears at the time of fever and can be easily missed.