Medications to Treat Inflammatory Disease
Changes in the recent decade to approach and treatments available have been considerable with emergence of potent immunosuppressive agents used early in the disease course.
More information about the medications and their use in practice is available in pmm-nursing.
Exposure to oral corticosteroids should be minimized as they can cause severe side effects and less corticosteroid exposure has been enabled through increasing use of intra-articular corticosteroids and early use of disease-modifying anti-rheumatic drugs (DMARDs) with methotrexate (MTX) being the agent of choice. Intra-articular corticosteroids are highly effective, safe and is first-line treatment for oligo-articular JIA; young children require sedation or anaesthetic for the procedure, although in the older child inhaled analgesia (e.g., nitrous oxide) may be used. Pulsed intravenous methylprednisolone is often used to induce remission at disease onset, during flares of polyarthritis or in those with features of systemic-onset JIA or multisystem disease, and is a useful bridging agent whilst starting MTX therapy. Topical corticosteroids (eye drops) treat uveitis although systemic immunosuppression including MTX is often used if uveitis does not respond to eye drops alone. Periocular injections can be given to control uveitis. Where systemic corticosteroids are used then optimizing dietary intake of calcium and vitamin D is important; the role of calcium and vitamin supplements or bisphosphonates to reduce the risk of osteoporosis is unclear.
Non-steroidal anti-inflammatory drugs (NSAIDs) can relieve symptoms in the short term but are not disease modifying; there are concerns about long term risk (including renal and cardiovascular disease) and their use for short term only is advocated and where possible use of sugar-free preparations to reduce the risk of dental caries.
Methotrexate (MTX) is the most widely used DMARD for JIA - and is effective in both joint disease and uveitis. However MTX is slow to take effect (often 3 months) - joint injections or Intravenous or oral steroids) may be used as bridging agents. MTX is usually started immediately after the diagnosis is confirmed in any subtype of JIA other than oligoarticular JIA; MTX is used in oligoarticular JIA if there is failure to respond to intra-articular corticosteroids. MTX is given once a week (by tablet or liquid) and also by subcutaneous (SC) injection which can be delivered and administered at home. Nausea, which can be anticipatory, is often the main reason for stopping MTX treatment or switching to other drugs including biologics. Other side effects are uncommon (e.g., cytopenia or abnormal liver function tests). Serious complications (including malignancy and infertility), have not been reported to date. MTX is a teratogen so appropriate advice regarding contraception is needed.
Other DMARDs, including sulphasalazine, azathioprine and cyclosporin can be useful but are less effective than MTX. Gold, penicillamine and hydroxychloroquine are now rarely used in JIA (but hydroxychloroquine may be useful in JSLE - especially to help skin disease). Sulphasalazine can be useful in oligoarticular JIA or enthesitis related arthritis. In the child with severe disease, who is resistant to or intolerant of MTX, biologic therapies are often used although for many parts of the world, access to these is very limited due to their high cost. The emergence of biosimilars is likely to result in lower costs and therefore improve access to effective treatments for more children although there are concerns about safety and efficacy. Cytotoxics (such as cyclophosphamide and mycophenolate mofetil) are used to treated severe JSLE and vasculitis.
Biologic and novel therapies selectively block effects of pro-inflammatory cytokines and there is evidence of dramatic and sustained improvement in disease control. Their use in JIA and other multisystem diseases is increasing. Long-term safety and efficacy data is important to address concerns about infection risk, impact on fertility and malignancy risk long term. There are many registries and cohort studies in progress to collect this data. These drugs are expensive and guidelines for their use exist. For those few children with severe refractory disease failing to respond to cytokine modulators, a further option is T-cell depletion coupled with autologous haematopoietic stem-cell rescue; this procedure is limited to specialist centres and needs careful selection of patients.
Monitoring and advice: Regular blood tests to monitor the efficacy and safety of immunosuppressive agents are essential. Baseline investigation prior to starting immunosuppression include tests to exclude infection. Vigilance regarding infection is important, especially as the classical symptoms and signs may not be apparent, and urgent referral is warranted if infection is suspected. Patients and families need to know to avoid live vaccines and pregnancy when on MTX or biologics and other immunosuppressives, especially if also on systemic corticosteroids. Families need to know when to seek prompt medical care if the child is unwell and especially if they develop chickenpox or herpes zoster, as these can be life threatening. Varicella vaccination should be considered in all patients with incident JIA who are non-immune and before immunosuppression is started. In the young person taking MTX, education about contraception (MTX is a teratogen) and avoidance of excessive alcohol consumption is essential.
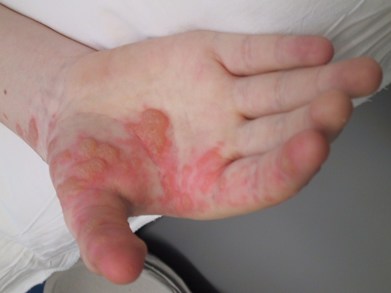
The photograph shows herpes zoster infection (shingles) in a child who is immunosuppressed.
More information about the medicines and how they are used in specialist clinical practice, is available. These are exemplar guidelines and it is likely that details of practice will vary between specialist centres.
https://starship.org.nz/guidelines/immunosuppression-infection-and-immunisation-in-rheumatology


