Juvenile Systemic Lupus Erythematosus
Juvenile Systemic lupus Erythematosus (JSLE) is rare but is more common in certain ethnicities (e.g., Asian, Black African, First Nations [North America, Australia and New Zealand]) with a predominance of girls affected in the adolescent group and a more equal sex distribution in young children. Arthritis is common in JSLE, as 80% of JSLE patients will experience it during their disease course. The arthritis of JSLE is usually polyarticular, often the swelling is symmetric, and not acutely painful. There are many possible extra-articular features and so children may present to health care in different ways.
Common presenting symptoms of JSLE:
- Skin - Malar rash (photosensitivity), Alopecia, Vasculitic rashes, Raynaud’s phenomenon. Changes can vary, be subtle and can be easily missed.
- Arthritis - Polyarticular (small joints hands and feet), swelling and stiffness.
- Systemic features - Fatigue / Fever / Weight loss / Oral ulcers.
- Pleuritis/pericarditis (e.g., chest pain, shortness of breath).
- Central nervous system (e.g., headaches, seizures, psychosis).
- Lymphadenopathy.
- Hepatosplenomegaly.
- Hypertension, peripheral oedema, facial puffiness (periorbital oedema).
Laboratory findings:
- Anaemia (may be haemolytic with positive red cell autoantibodies).
- Leukopaenia, lymphopaenia, thrombocytopaenia.
- Blood and or protein in the urine.
- Elevated liver enzymes (AST, ALT).
- Elevated kidney function tests (blood urea nitrogen, creatinine).
- Decreased complement components C3 and C4.
- Positive antinuclear antibody.
- High titre positive anti-double stranded (ds) DNA antibody.
- Positive autoantibodies to extractable antigens (anti-Ro [SSA]; anti-La [SSB]; anti-Sm; anti- RNP) and positive antiphospholipid antibodies (anti-cardiolipin, lupus anticoagulant).
Drug-induced JSLE can develop from the use of anti-convulsants, oral contraceptives, minocycline and many other medications.
The medical management of JSLE is complex and requires specialist supervision, with nearly all patients requiring hydroxychloroquine, corticosteroid and potent immunosuppressive medications (including cyclophosphamide or mycophenolate mofetil). Investigations before starting immunosuppression are important to exclude infection and malignancy. Patients often require anti-hypertensives, anticoagulation (related to antiphospholipid syndrome), medications to control dyslipidaemias and prevent osteoporosis (e.g., calcium & vitamin D supplementation). More information about management is given in PMM-nursing.
Neonatal lupus (NLE) occurs in neonates as a result of fetal exposure to maternal anti-SSA/Ro antibodies. The mother can carry a diagnosis of SLE or Sjogren’s syndrome, but other times is asymptomatic and unaware of antibody status. This syndrome is due to passively acquired maternal IgG antibodies. The most serious complication is injury of cardiac conducting system tissue during fetal development, resulting in heart block, progressing to hydrops fetalis in the most severe cases. Endomyocardial disease can occur in addition to or apart from conduction defects. Other clinical manifestations occur, including skin rash involving face and scalp, trunk and extremities. Haematologic abnormalities such anaemia, leucopenia, and thrombocytopenia can occur, with thrombocytopenia being most common. Other clinical features can occur (e.g., hepatitis, macrocephaly), and a neonate with NLE should be evaluated by a paediatric rheumatologist and the mother also assessed by a rheumatologist. Congenital heart block requires evaluation in consultation with neonatal care experts and paediatric cardiology experts. Complete heart block is irreversible. The risk of complete heart block is highest in children born to women with a previous child with NLE. Therapeutics such as glucocorticoids and intravenous intraglobulin are utilized at the advice of expert consultation. If there is no injury to the cardiac conducting system, all other symptoms tend to fade away as the infant clears maternal antibodies, around 6-8 months of age. Useful references about NLE:
https://doi.org/10.1016/B978-0-12-820583-9.00003-8
https://doi.org/10.3899/jrheum.201338
The following resources are useful to demonstrate skin changes of JSLE and NLE:
Welcome to Skin Deep - Skin Deep (dftbskindeep.com)
https://www.nottingham.ac.uk/research/groups/cebd/resources/skin-of-colour/index.aspx
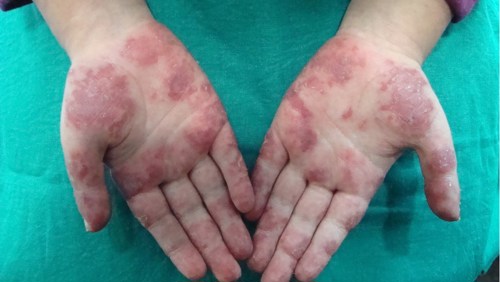
The photograph below shows skin vasculitis in JSLE
Suggested Further Reading


