Tuberculosis
Tuberculosis (TB) needs to be suspected in endemic areas or children who have had contact with family from an endemic area. Children with TB might appear well or have systemic symptoms (night sweats, poor growth or weight loss). Inflammatory markers may be elevated and there can be anaemia or chronic disease. The joint may not be hot or red but joint damage can be indolent with chronic abscess and sinus formation. TB should also be considered in a child who is unwell with a swollen joint, and especially if they are immunosuppressed due to disease or treatment. Children with TB often have co-existent HIV (Human Immunodeficiency Virus). TB may also be a cause of chronic joint pain in otherwise well looking children with families from endemic areas; the diagnosis rests on clinical suspicion, Mantoux or positive TB testing using QuantiFERON® gold, followed by synovial biopsy.
Atypical mycobacteria can cause infection and can be acquired from pets (ask about reptiles and tropical fish at home).
Infection is often indolent, leading to significant diagnostic delay. Spinal lesions are common with pain or limp. Vertebral collapse may result in kyphosis. Paraplegia can occur due to spinal cord compression from vertebral involvement or abscess (Pott's disease).
The radiographs below show vertebral collapse (arrowed) due to TB of the spine.
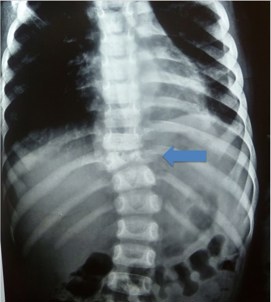
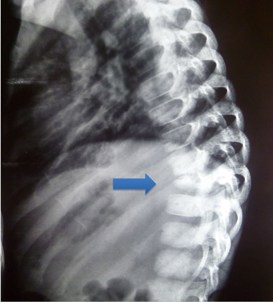
TB Infection may involve the metaphysis of the femur, tibia, skull and small bones of hands and feet (i.e., dactylitis). TB osteomyelitis can be associated with tuberculous arthritis, an overlying cold abscess and or sinuses. Dactylitis (below) usually presents as painless or mildly painful swelling mostly involving the proximal phalanges or the metacarpal bones.
TB osteomyelitis is most commonly a single focal process in the immune-competent host. TB arthritis is often gradual with swelling, joint restriction and pain. Phlycten is an allergic conjunctivitis and may indicate mycobacterial infection.
A reactive arthritis to mycobacterial infection is also observed (called Poncet's disease) and thought to be due to a hypersensitive immune response to tuberculoprotein; this is similar to erythema nodosum occurring in the skin with active TB. Poncet's disease predominantly occurs in young adults and children and usually presents with a fever of 3-16 weeks duration followed by an acute / subacute polyarthritis. Poncet’s disease tends to be a symmetrical oligoarticular arthritis of predominantly the large joints (the knees are most commonly involved). Cervical and axillary lymphadenopathy is a consistent finding. Poncet’s disease is more commonly associated with active extra pulmonary TB - notably that involving the lymph nodes. The diagnosis of Poncet’s disease is largely clinical and is made by excluding other causes of polyarthritis in a patient with documented active TB. The arthritis resolves on treatment with anti-tuberculosis therapy.
The diagnosis of TB is suspected from the clinical presentation, positive Mantoux test and radiograph changes. Definitive diagnosis relies on culture of the organism - open biopsy or fine needle aspiration of bone, or synovial fluid aspiration and synovial biopsy. DNA analysis of synovial fluid may give rapid diagnosis but may not always be available. In areas with a high prevalence of multidrug resistant Tuberculosis (MDR TB), culture and sensitivity testing should be routine. There is risk of co-existent HIV with TB and appropriate HIV testing is needed. The differential diagnosis includes bacterial and fungal infection and bone tumours. Differentiating between TB, septic arthritis and JIA can be difficult and the table below gives helpful pointers.
The photograph below shows a swollen index finger involving the proximal interphalangeal joint and due to atypical mycobacteria in a child on immunosuppressive treatment.
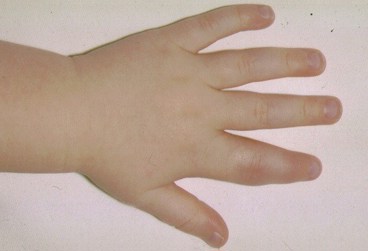
Differentiating between TB, septic arthritis and Juvenile Idiopathic Arthritis (JIA)
|
Mycobacterial/TB |
Septic arthritis |
JIA |
|
A history of contact may be present. |
Child likely to be unwell and in severe pain with fever. |
May be extra-articular features (rash, uveitis). |
|
Invariably a monoarthritis. Spine is often involved. Multi-ostotic forms noted. |
Monoarthritis, any joint. |
Pattern of joint involvement is variable. Any joints may be affected, any number. |
|
Can present with systemic symptoms. Joint features are typically a single swollen joint. Extra-articular features such as erythema nodosum, uveitis, red eye (phlycten). Positive Mantoux test. |
Joint pain severe and joint or limb held immobile. Often non-weight bearing. Patient systemically unwell with fever and malaise. |
Joint symptoms often variable with diurnal variation and by definition, last > 6 weeks. |
|
Full (Complete) blood count may show leucocytosis with mild lymphocytic predominance. ESR is raised |
Raised white cell count and acute phase reactants. May be febrile. |
May be normal acute phase reactants (ESR and CRP) and white cell count. |
|
High synovial fluid white cell count. Culture may grow mycobacteria. Synovial biopsy shows caseating granulomas. |
Very high synovial fluid white blood cell count. Organisms cultured. |
Moderately raised synovial fluid white cell count but sterile. |


